On Wednesday night I called my good buddy Kevin Russell and asked him: what do you actually want to know? What do you think people are asking? So I let him ask whatever he wanted — what he was actually thinking.
I wanted this to feel like you're sitting across from me. I want to update people, but I also want this to be educational. I want people to understand what it's like to go through the surgery I had.
Kevin asked. I answered. If there's something I missed, drop it in the comments and I'd love to answer it.
How did the surgery actually go?

My neurosurgeon reported that the surgery went exactly as planned, exactly as intended. We couldn't have asked for a better outcome.
Specifically: no obstructions at the foramen magnum, no CSF leakage, and no complications. He also told me my bone was exceptionally thick. Must be all the milk I've drunk over the years.
"The patient was brought into the operating room. He was intubated and placed under general anesthesia. Baseline neuromonitoring was obtained… Neuromonitoring was stable to actually improved. A posterior midline incision was planned from the inion to C2… His bone was exceptionally thick. A C1 laminectomy was performed about 2.75 cm wide… There was no obstruction at the outlet of the fourth ventricle. We then took a great deal of time to cauterize and shrink the tonsils up close to the foramen magnum… There was no CSF leakage from the dural suture line after it was complete. Valsalva did not induce any leak. He was moving all extremities before leaving the operating room. Complications: None."
Neurosurgeon · Operative Report · 2/26/2026
What was the tethered cord MRI about?
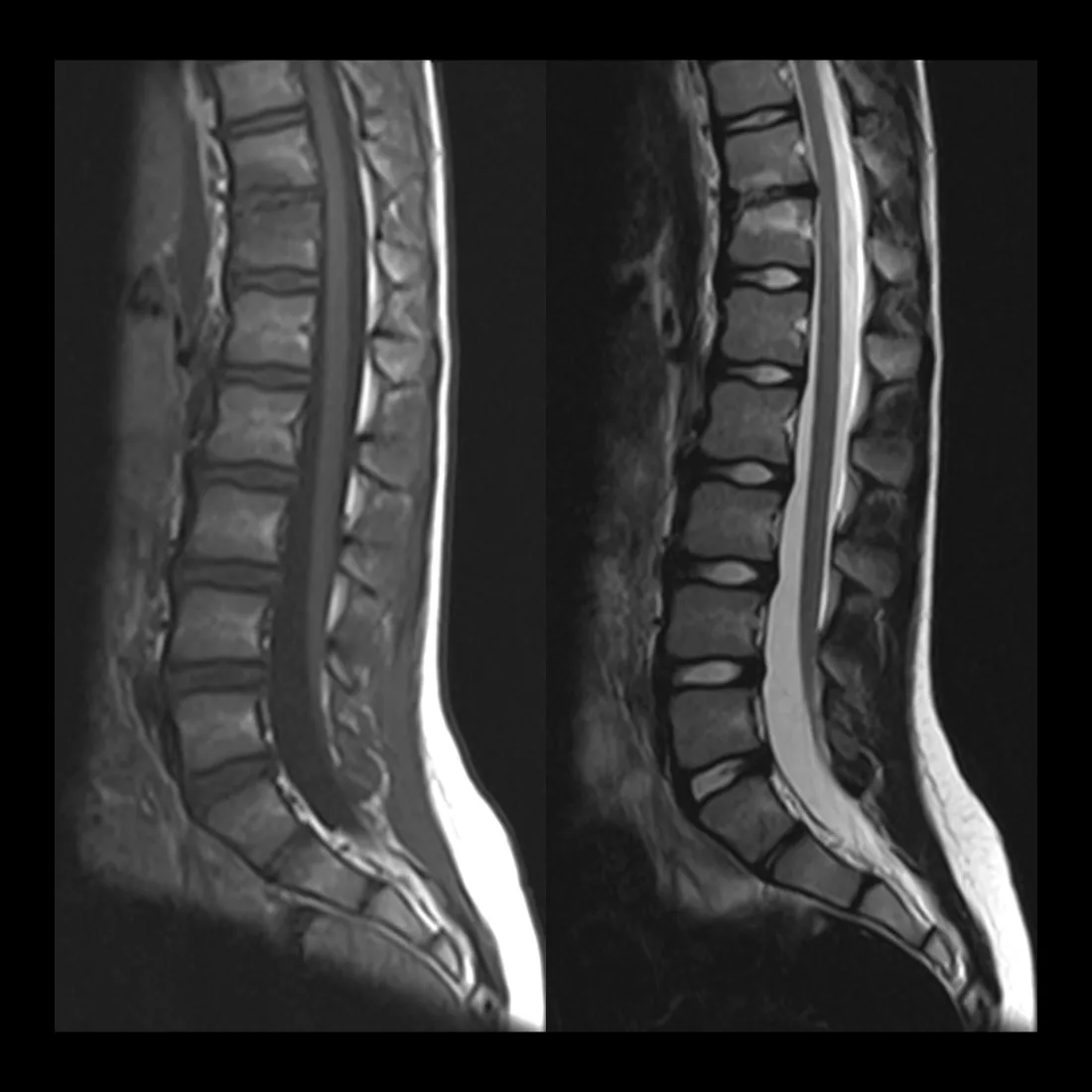
Before surgery, Dr. Lee wanted an MRI of my lower spine to check for a tethered cord, the idea being that if I had one, they could potentially do both surgeries at the same time. But VA insurance made it nearly impossible to turn that around before my surgery date.
So during my stay, they came back to me and said: since you're already here and everything is under the same VA referral, we'd like to get that MRI now. They were seeing symptoms that could be coming from a tethered cord, and if that was the case, they wanted to operate. The MRI came back clear. No tethered cord.
The spinal cord isn't fixed in place. It's designed to move. When you bend, sit, or stretch, the cord shifts slightly within the spinal canal. That mobility is by design.
A tethered cord is what happens when something anchors it. Scar tissue, a fatty filum, a structural abnormality. Whatever the cause, the cord gets held in place when it shouldn't be. Tension builds along nervous tissue that has no tolerance for it.
The symptoms accumulate slowly. Leg weakness, bladder dysfunction, back pain nobody can explain. Patients often spend years being evaluated for everything except the actual problem. Treatment is surgical: they find what's holding the cord, release it, and give the nervous system room to recover.
So what does the pain actually feel like?

Pretty tolerable, honestly. The resident set me up well — she told me the first few days would be very painful. She bolded the word "painful." Then I'd feel a whole lot better. She was right.
Once they brought in a pain management team and started the Ketamine and Lidocaine drip, things improved significantly. Then they switched me to Oxy after 48 hours.
The car ride home was rough. Pillows, blankets, neck pillows, even my mom's vest. Anything we could find went to support my neck. By the tail end I was holding my head to keep it from moving. I felt every bump, every lane switch, every turn. The roads in Illinois are terrible for pain management.
Anything that spiked my intracranial pressure shot the pain up, laughing, coughing, any of that.
Now that I'm home, here's where things actually stand with pain: light headache across the front, feels like someone stabbing down on the top of my head, and the stitches in the back feel like they're about to burst. That last one has been the most constant.
Four medications holding it together: Oxy, Gabapentin for nerve pain, Methocarbamol for muscle spasms, and Tylenol. We tapered off over about a week. Friday was my last day on Oxy. The muscle relaxers, nerve blockers, and Tylenol are staying on for the next few weeks, and I can definitely feel the difference without the narcotics. But I'm managing.
The surgery required dissecting the muscles at the back of the neck away from the spine to access the skull and C1. Those muscles are now healing back into place over a repaired site that includes staples, a dural patch, and new bone margins. The pressure and pulling sensation, that feeling like the stitches are about to pop, is the tissue healing and the nerves in the scalp regenerating. It's uncomfortable, but it's the incision doing exactly what it's supposed to do.
The muscles at the back of the neck weren't moved aside during surgery. They were cut. Those are load-bearing muscles responsible for stabilizing and supporting the head.
In the days after surgery, those muscles are healing and haven't regained their strength. The head, which weighs roughly ten to twelve pounds, is sitting on a repair site that isn't ready to bear full load yet. Every bump transfers directly to that site, and every lane change creates lateral movement the muscles can't yet resist.
By the end of that drive I was holding my own head with my hands to keep it from moving. That's not dramatic. That's just the physics of a healing neck with no shock absorption left. The roads in Illinois didn't help.
What's the part of recovery you didn't expect?
Going into surgery, I thought my two biggest problems were going to be pain and train of thought. Train of thought is pretty spot on, but it's really the energy levels and how much the medication affects me that's hit me hardest. I've really been yearning to get off these drugs. I just didn't know how bad being medicated would feel. And it's terrible.
I also didn't think I'd have as hard a time walking as I did. But honestly, I'm recovering a lot faster than I thought I ought to be. A lot of the clothes I packed were just for laying around the house, but I went to church on Sunday and have been doing other stuff I didn't think I'd be able to do. So I'm very thankful.
My mom and I have been laughing about this video where a guy in a wheelchair at Walmart, paralyzed, using a voice box, rolls around with his mom and types out: She drugs me to keep me this way. That's really what I've been feeling.
When you laugh or cough, you're doing what's called a Valsalva maneuver. Your body bears down and it spikes the pressure inside your skull. The surgery created more space and restored CSF flow, but the brain is still healing. So right now, that pressure spike still finds you. It settles as recovery progresses.
The cerebellum, the part of the brain that was being compressed, does a lot more than control balance and coordination. It plays a role in regulating energy, attention, and processing. When you decompress it and restore CSF flow, the brain begins a recalibration process. That takes an enormous amount of energy. Add nine medications on top of it and the fatigue makes complete sense.
How are you sleeping?
Since surgery I've had to sleep at a 30-degree angle, which is pretty annoying given the amount of pillows it takes to make that work. I've also been going to sleep with an ice pack behind my head, one of those recirculating ones that pulls cold water from a gallon jug I fill up before bed. That's been really helpful.
Honestly, I've been sleeping a whole lot. My sleep schedule has been pretty messed up, going to bed around two, sleeping until noon, catching an afternoon nap around four. I'm hoping to transition to a better schedule this coming week.
The surgery involved removing bone at the base of the skull and the top of the cervical spine. Lying flat in the early weeks increases pressure at the surgical site and puts strain on everything that was just repaired. The 30-degree angle keeps the head elevated enough to let fluid drain properly and takes the pressure off the incision while it heals.
What are you actually capable of right now — how long does recovery take?

I walked around the neighborhood today. Walker is gone, doing stairs on my own. It was 56 degrees and sunny, which felt great. I didn't feel the best afterwards and ended up with a headache, but it was worth it.
Still no driving, still can't work out, still no running. Every day I'm able to do a little more.
| Can't Do | Until | Can Do |
|---|---|---|
| Drive | Until cleared | ✓Walk the neighborhood |
| Lift more than 10 lbs | 6 weeks | ✓Stairs solo |
| Swim / hot tub / tub bath | 6 weeks | ✓Daily shower |
| Bend over | 6 weeks | ✓Get outside in good weather |
| Run or work out | Until cleared | ✓Gradually increase walk distance |
| Wear hats / caps / bandanas | Mar 16 appt | ✓No headwear needed (yet) |
| Hair products | 6 weeks | ✓Baby shampoo + ends-only conditioner |
| Dye hair | 3 months | ✓Wash hair daily |
| Dental work / cleanings | 3 months | ✓Tylenol + prescription meds |
| Aspirin / ibuprofen / Advil | 2 weeks | — |
| Smoke | Permanently | — |
| Long car trips without stops | While recovering | ✓Stop & walk every 2 hrs |
Can you turn your head yet?
Turning my head has gotten easier by the day. I'd say I'm able to turn in either direction about 45 degrees, and looking up and down has also improved a lot. Not back to 80 degrees yet, but we're definitely working in that direction.
The range of motion does change like the stock market, throughout the day and from day to day. Some days better, some days worse. But in general, it's definitely trending up.
Are the tremors gone?
The tremors are gone. They went away while I was still in the hospital.
The cerebellum is the part of the brain responsible for coordinating movement. When it's been compressed for an extended period, as mine was by a 15mm herniation, the signals it sends to your muscles become unreliable. After surgery the tremors showed up more consistently, but only for the first few days. Then they stopped. The surgery decompressed the cerebellum and restored CSF flow. The nervous system didn't need time to learn something new. It needed the obstruction removed. Once it was, the tremors resolved on their own.
What about the things that brought you to surgery — swallowing, balance, thinking clarity?
Have I noticed improvement from the symptoms that brought me into surgery? Not really right off the bat. I kind of jumped from the pan into the fire. This surgery is about lifelong benefits, not immediate relief. Balance is improving from where it was right after surgery, and swallowing hasn't been as much of an issue as I expected. PT is going to help a lot with both.
Thinking clarity has been rough, but that's mostly the medication being disruptive. That's something I want to dive deeper into in a future post.
The short version is that recovery from this surgery isn't measured in days or weeks. It's months. Three to six months is where many people notice relief from headaches and pressure symptoms. Balance, swallowing, and coordination can lag behind. Six to twelve months is where meaningful neurological improvement tends to happen. I'm early. I'm moving in the right direction.
Cerebrospinal fluid isn't static. It circulates continuously around your brain and down your spinal cord, cushioning, regulating pressure, and clearing waste. When the cerebellar tonsils herniate through the foramen magnum the way mine did, that circulation gets obstructed. Pressure builds and the system backs up.
The surgery created room. The C1 laminectomy widened the exit, the duraplasty expanded the dural sac, and the tonsils were cauterized back up toward the foramen magnum. The symptoms didn't come from nowhere. They came from a nervous system under sustained hydraulic pressure. Restoring flow doesn't flip a switch, and the nervous system adapts over weeks and months. But the pressure is gone, the repair is in place, and the rest is just time.
Opioids suppress the central nervous system. That's how they manage pain, but it's also why everything feels slower and foggier. Attention, processing speed, word finding, all of it gets dampened. That's not a post-surgical cognitive change. That's the drugs. As I taper off and things clear out, the picture will become a lot more accurate.
Spiritually, how are you feeling?
Honestly, this surgery has given me a lot of downtime, and I'm not good with downtime. It's pulled me away from Nashville, from Stonebridge, from my community group, and those things are what keep me anchored. Being away from Nashville has distanced me from that community, and I feel it.
One thought I've been wrestling with is that the devil didn't care what Job went through. He only cared about the sin Job was tempted by in the middle of it. I've been doing a lot of reflection on that.
Emotions are hard to regulate on nine medications. But I do think this trial will make me stronger. I'm still thankful for it. Still fighting the good fight.
"The devil didn't care what Job went through. He only cared about the sin Job was tempted by in the middle of it."What does the scar look like?
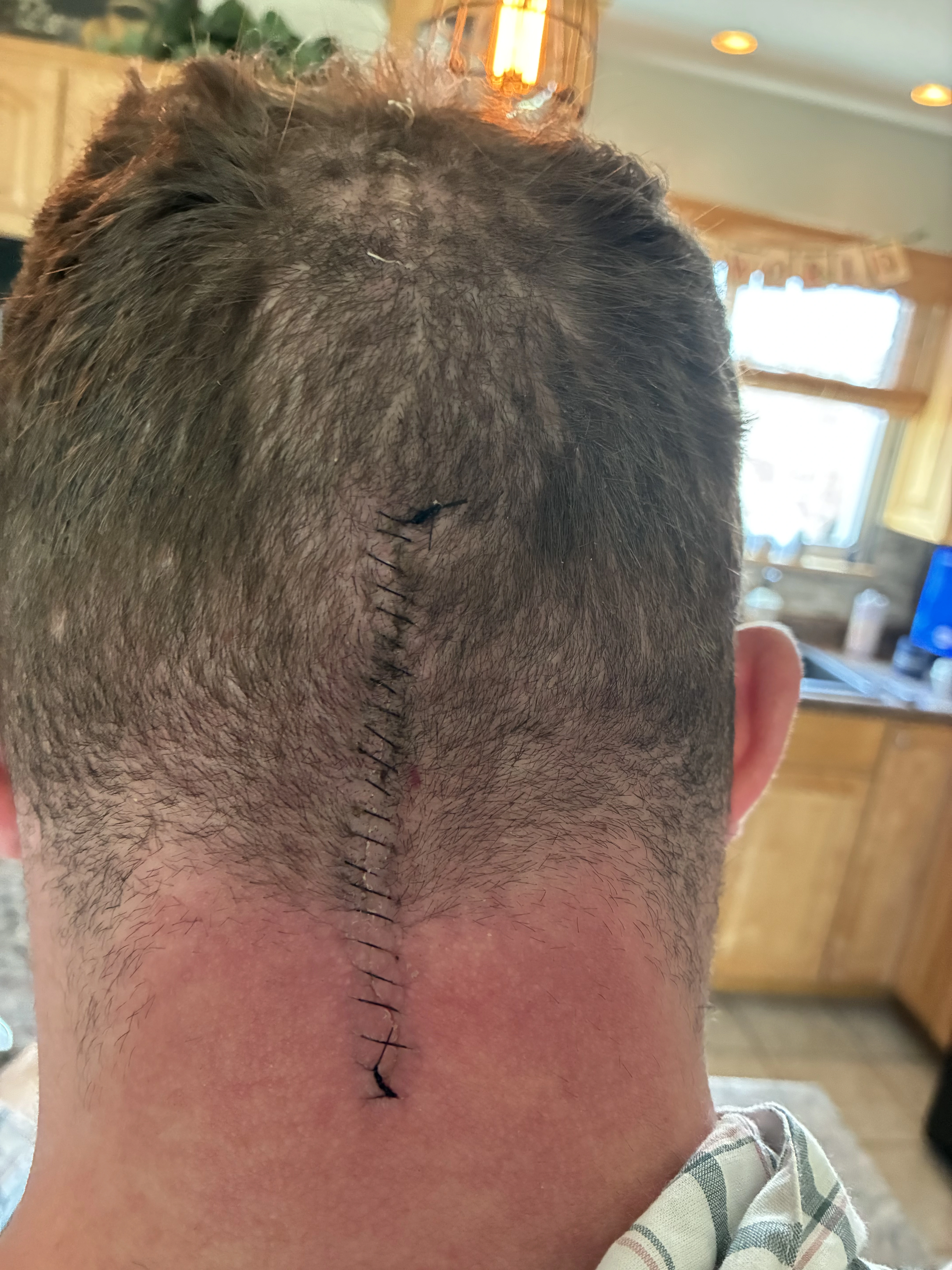
Honestly, the scar looks amazing. The incision is incredibly clean, the sutures are evenly spaced, the closure is tight and well aligned. It's wild how precise it is.
I went into surgery thinking I'd have one scar. I ended up with four. Two on the sides of my head from the Mayfield clamp that held my head in place during surgery, one on top where they harvested the patch for the duraplasty, and the main incision at the base of my skull.
Yes, but not yet, and not without clearance. Once the incision is fully closed and the sutures are out, typically around the six-week mark, gentle scar massage becomes part of the recovery. The technique starts at the edges, not the scar itself. Small circular motions in the surrounding tissue keep it from binding down as collagen forms. As the tissue matures, you work closer in.
It breaks up early adhesions, keeps the tissue mobile, and helps the nerves in the scalp recalibrate as they regenerate. That tight, pulling sensation around the incision, the one that feels like the stitches are about to pop, that's exactly what consistent massage is working against once the healing is far enough along to allow it.
The site involves the skull, the dura, and the top of the cervical spine. Timing matters. Don't start without your surgeon's go-ahead.
What's Coming Next
First things first, I'm getting my stitches out on the 16th. Still here in St. Louis with my family until after Easter, and honestly, I'm looking forward to every bit of this time with them. Hoping to see my little cousins on Friday. We'll also be continuing to taper off the nerve blockers and other medication, so that's ongoing.
send me
Share your thoughts